In this Journal Club
5-Point Summary
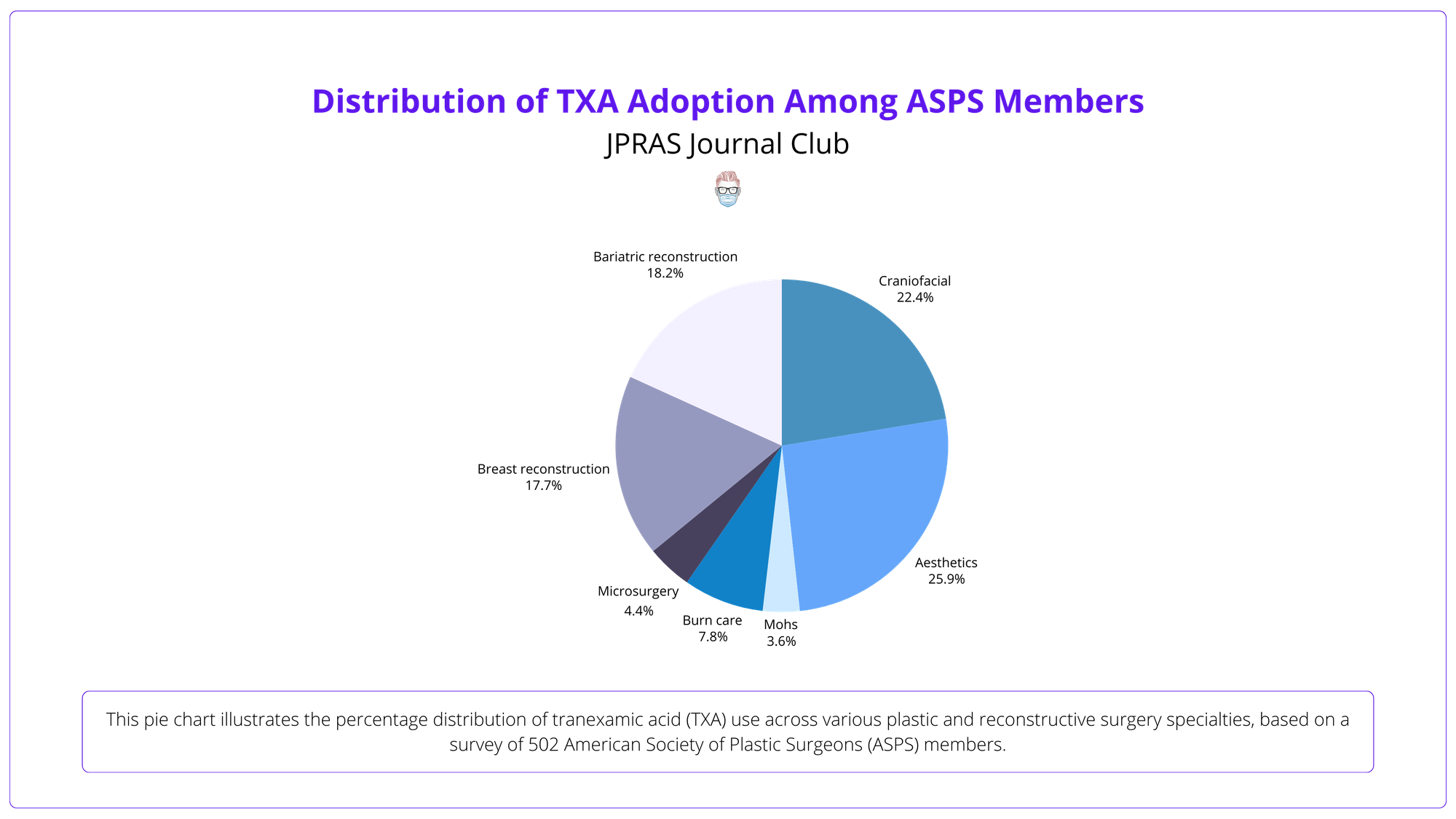
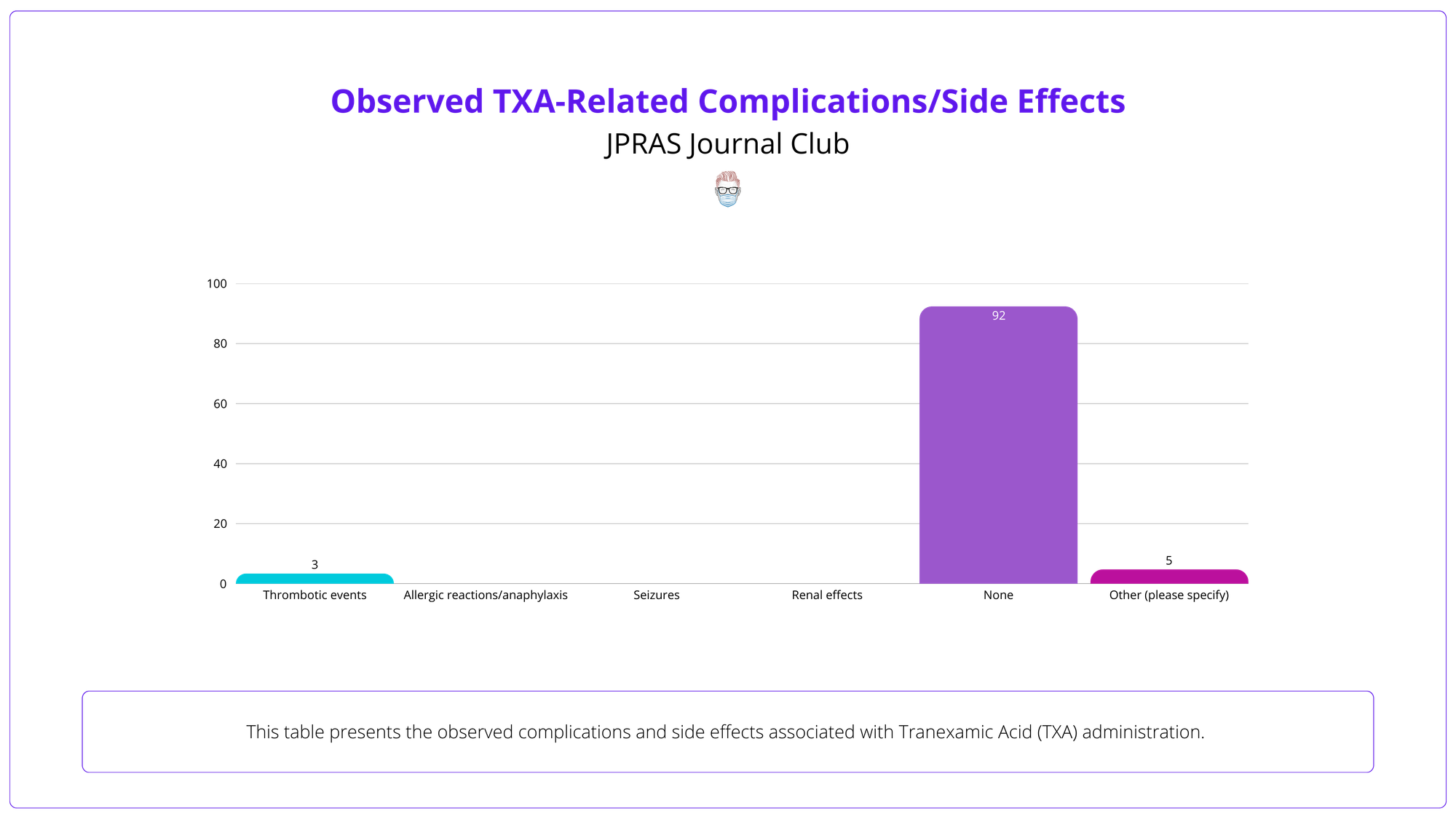
TXA is widely used among ASPS members, especially in aesthetic (90.3%) and craniofacial surgery (78.2%), with 92.4% reporting no complications.
4-Key Findings
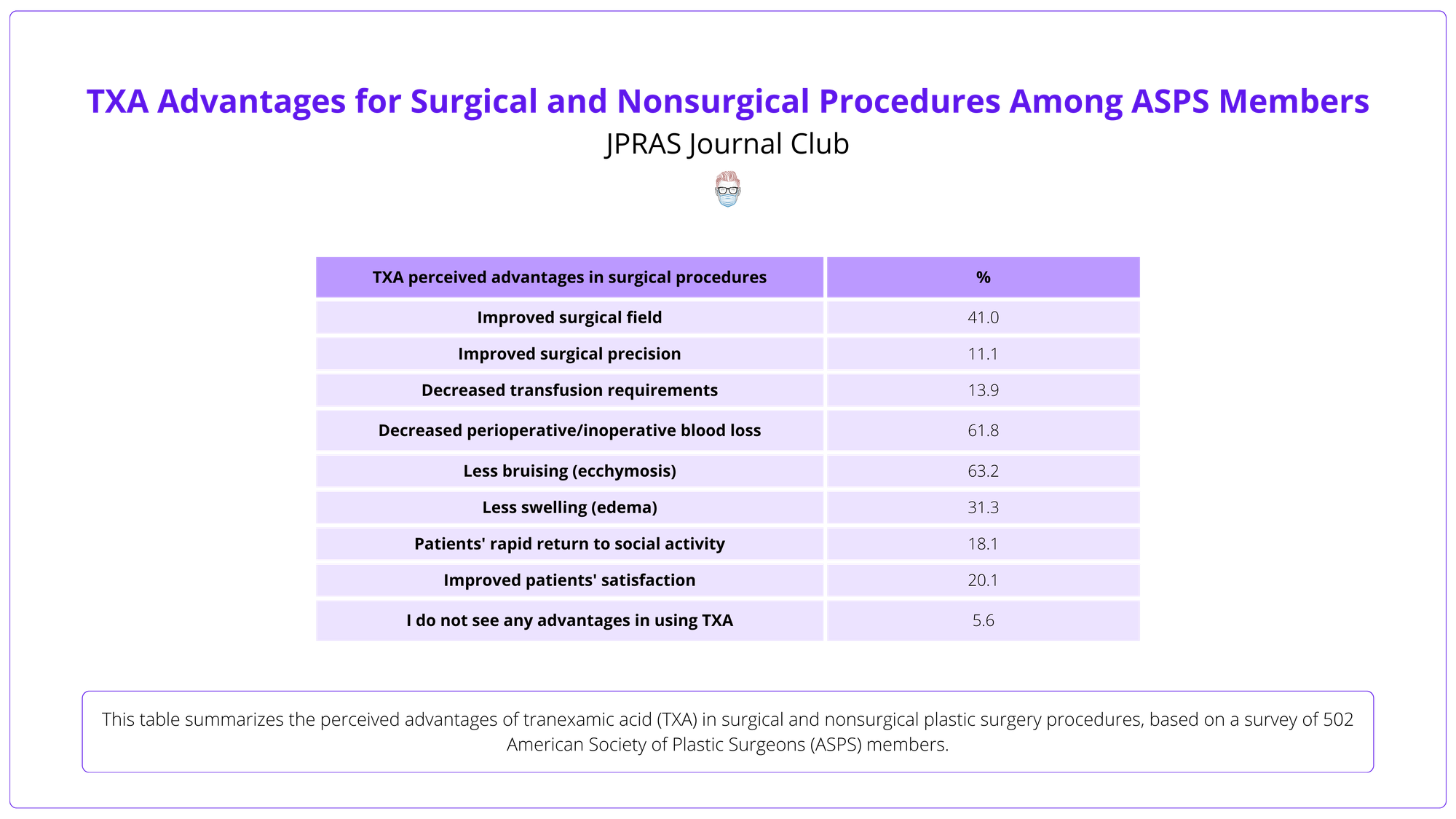
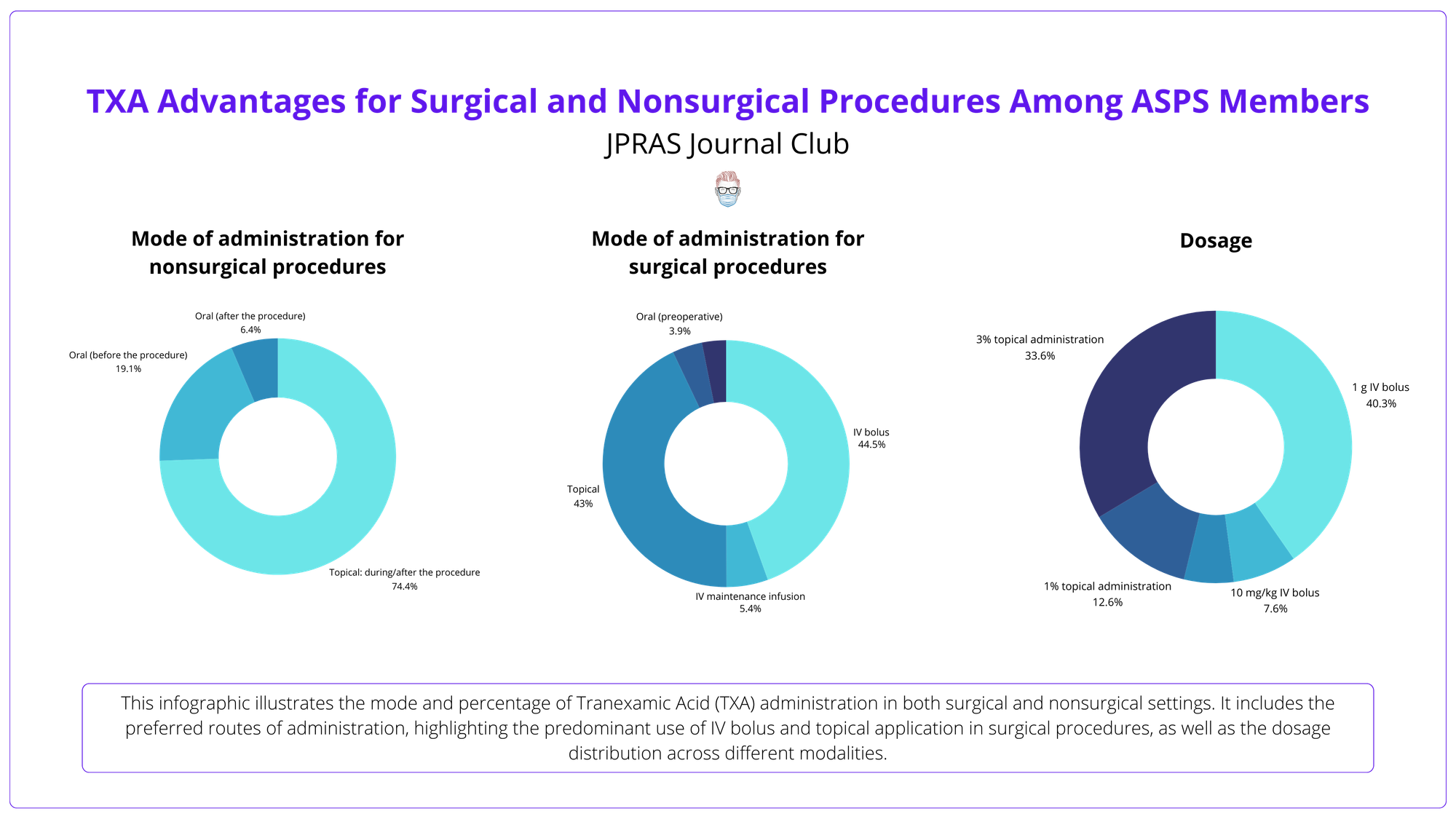
TXA is common in facelifts (83.6%) and rhinoplasty (55.0%), with 61.8% reporting less bleeding and 63.2% less bruising. Popular methods include 1 g IV bolus (43.2%) and 3% topical solution (36.0%).
3-Critiques
A 21% response rate risks selection bias, potentially overrepresenting TXA users. Detailed outcomes are lacking data for specific procedures. Self-reported complications may be skewed by recall bias.
2-Practical Takeaways
TXA (1 g IV or 3% topical) reduces bleeding and bruising in facelifts and rhinoplasty. Topical TXA offers a safe, localized option for high-bleed surgeries.
1-Recommended Reading
Brown et al.’s meta-analysis (45 studies, 4,361 patients) confirms that TXA reduces blood loss in rhinoplasty and craniofacial surgery, supporting standardized protocols.
Primary Contributor: Hatan Mortada, Educational Fellow
Verified by JPRAS✅
Rohrich et al report widespread use of TXA among ASPS members with very low numbers reporting complications. There is good evidence for TXA use in trauma; however, elective breast and aesthetic surgery data is developing and will require further focussed research with validated outcome measures to enable standardised approaches to dosage, delivery route and timing. Congratulations to Rohrich and co-authors for publishing this work and raising awareness of the current trends in TXA use.
Adam Reid, JPRAS Editor
5 Point Summary
This study explores the use of tranexamic acid (TXA) among American Society of Plastic Surgeons (ASPS) members, highlighting its widespread adoption, preferred administration methods, and safety profile in plastic surgery.
1️⃣ Hypothesis: TXA is increasingly utilized in plastic surgery with varying practices, but standardized guidelines are lacking.
2️⃣ Method: A survey of 502 ASPS members assessed TXA use across procedures, administration protocols, and perceived benefits.
3️⃣ Results: TXA is most common in aesthetic (90.3%) and craniofacial surgery (78.2%), with 92.4% reporting no complications.
4️⃣ Conclusion: TXA is effective and safe, but administration varies widely, necessitating standardized protocols.
5️⃣ Implication: Evidence supports broader TXA adoption, though further research is needed for specific procedures.
4 Key Findings
The survey reveals TXA’s prominence in specific fields, its benefits in reducing bleeding, and a reassuring safety profile.

3 Critiques
While comprehensive, the study has limitations in scope, depth, and generalizability.
1️⃣ Response Rate: The 21% response rate (502/2,390 members) may introduce selection bias, potentially overrepresenting TXA users.
2️⃣ Outcomes: Lack of procedure-specific outcome data limits insights into TXA’s efficacy for individual surgeries like abdominoplasty.
3️⃣ Self-reporting: Self-reported complication rates may underreport adverse events due to recall bias or reluctance to disclose.

2 Practical Takeaways
TXA offers actionable benefits for surgeons, particularly in aesthetic and craniofacial fields.
1️⃣ Efficacy: Surgeons can confidently use TXA (e.g., 1 g IV or 3% topical) in facelifts or rhinoplasty to reduce bleeding and bruising.
2️⃣ Safety: Topical TXA’s low systemic absorption makes it a safe option for localized effects, minimizing risks in high-bleed procedures.
1 Recommended Reading
Brown et al.’s meta-analysis (45 studies, 4,361 patients) confirms that TXA reduces blood loss in rhinoplasty (high certainty) and craniofacial/burn surgery (moderate certainty), urging standardized outcome measures.
Read the Article

